In the realm of sleep disorders and auditory disturbances, the intricate link between sleep apnea and tinnitus has become an area of growing interest among researchers and healthcare professionals. Tinnitus, often described as a ringing, buzzing, or humming sensation in the ears, can be a perplexing and disruptive condition on its own.
When coupled with sleep apnea, a disorder characterized by breathing interruptions during sleep, the impact on overall well-being can be profound. This article delves into the correlation between sleep apnea and tinnitus, shedding light on the complexities of these conditions and exploring potential connections.
Unmasking Sleep Apnea
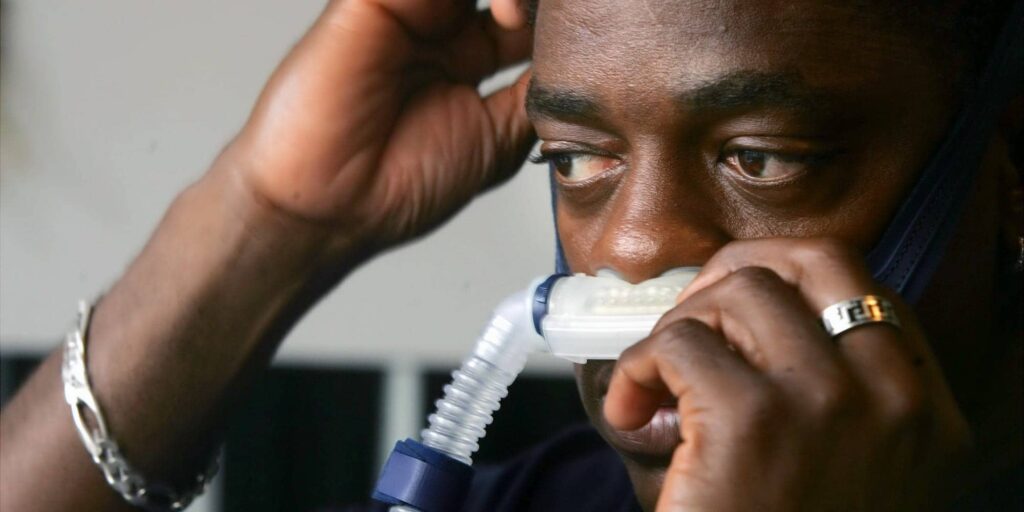
Sleep apnea is a sleep disorder marked by recurrent pauses in breathing during sleep. These pauses, known as apneas, can last for seconds to minutes and may occur multiple times throughout the night. There are three main types of sleep apnea: obstructive sleep apnea (OSA), central sleep apnea (CSA), and complex sleep apnea syndrome, also known as treatment-emergent central sleep apnea (CSA-CSR). OSA, the most common form, occurs when the muscles at the back of the throat relax excessively, causing a blockage of the airway.
Sleep apnea is heterogeneous in multiple dimensions. There are different physiological risk factors that may have clinical relevance. However, assessing them is challenging. An approach to ascertain them using a simple model of ventilatory control has been proposed. It is based, however, on untenable assumptions.
There are limited validation data and reproducibility is not stellar. There are also different symptom subtypes. They have been found in multiple population-based and clinical cohorts worldwide. Symptomatic benefit from therapy is most marked in the excessively sleepy subtype. This group may also be the group at increased CV risk from obstructive sleep apnea.
People experience apnea when the muscles behind the throat relax. These muscles are responsible for providing support to the soft palate, uvula, tonsils, the side walls of the throat, and the tongue. During muscle relaxation, the air passage narrows or closes as you breathe in.
The absence of enough air can lower the oxygen level in the blood. Our brain senses this inability to breathe and briefly awakens us from sleep to ensure to reopen our airways. Although one might snort, choke, or gasp, one usually doesn’t remember it as this awakening is very brief. This pattern might recur five to 30 times or more each hour, all night, disturbing the ability to reach the deep and restful phases of sleep.
The Impact on Sleep Quality

While it’s known that sleep quality is important to overall health, there is no one definition of sleep quality set by sleep experts. Instead, sleep quality is often defined by sleepers themselves. There are many consistent factors sleepers report when evaluating whether or not they get quality sleep, including sleep disturbances, bedroom environment, and daytime sleep habits. Daytime experiences, such as feeling rested and restored after waking also influence whether or not someone feels they have had quality sleep.
The interrupted breathing patterns in sleep apnea can lead to fragmented sleep, resulting in excessive daytime sleepiness, fatigue, and irritability. The diminished quality of sleep can also contribute to a range of health issues, including cardiovascular problems, diabetes, and cognitive impairment.
Understanding Tinnitus

Decoding the Sounds of Tinnitus
Tinnitus is the perception of noise or ringing in the ears without any external source. It can manifest as a buzzing, hissing, clicking, or pulsing sound and may be constant or intermittent. Tinnitus can be a symptom of an underlying condition, such as hearing loss, exposure to loud noises, or neurological disorders. The relationship between sleep apnea and tinnitus lies in their shared impact on the auditory system.
The Interplay Between Sleep Apnea and Tinnitus
An Overlapping Symphony
Research suggests that individuals with sleep apnea may be more prone to developing tinnitus, and vice versa. The mechanisms linking these two conditions are complex and multifaceted. One proposed connection is the shared involvement of the autonomic nervous system and changes in blood flow to the inner ear. The intermittent oxygen desaturation during apneas in sleep apnea may contribute to oxidative stress, affecting the delicate structures of the inner ear and potentially triggering tinnitus.
Neurological Pathways and Brain Function
Both sleep apnea tinnitus can influence brain function, with disruptions in neural pathways and connectivity. The auditory system, central to the experience of tinnitus, is intricately connected to various brain regions involved in sleep regulation. Dysfunction in these areas may contribute to the onset or exacerbation of both sleep apnea and tinnitus.
Treatment Approaches
Addressing the Root Causes
Managing the interplay between sleep apnea and tinnitus often involves addressing the root causes of each condition. For sleep apnea, treatment options may include lifestyle modifications, continuous positive airway pressure (CPAP) therapy, or surgical interventions. Tinnitus management strategies can range from hearing aids and sound therapy to cognitive behavioral therapy and stress reduction techniques.
Collaborative Care for Comprehensive Solutions
Collaboration between sleep specialists, otolaryngologists, and other healthcare professionals is crucial for a holistic approach to managing both sleep apnea and tinnitus. Coordinated efforts can help identify and address underlying factors, providing patients with comprehensive solutions to improve sleep quality and alleviate tinnitus symptoms.
Conclusion
As we navigate the intricate relationship between sleep apnea and tinnitus, it becomes evident that these conditions are interconnected on multiple levels. Understanding the complexities of this interplay opens the door to more effective diagnostic and treatment approaches. By addressing both sleep apnea and tinnitus in a holistic manner, healthcare professionals can offer individuals a better chance at improved sleep quality and overall well-being.




